Known as a resourceful, strategic, and inspirational executive leader, Brian Woods, MD seeks to add value to any endeavor or relationship he enters. He graduated with his medical degree from the University of Texas Health Science Center at San Antonio and completed his anesthesiology residency at UT Southwestern Medical Center at Dallas. Dr. Woods also spent seven years in the United States Air Force, where he served as Chief of Aerospace Medicine and Flight Surgeon for the 28th Bomb Squadron, receiving the Meritorious Service Medal for his reengineering of the 7th Bomb Wing’s programs and services related mobility and manpower processing following 911.
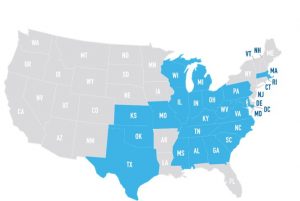
In 2007 he joined NorthStar Anesthesia in Dallas Texas and has helped lead and grow services in the company to over 1,000,000 anesthetics delivers per year in over 140 hospitals and ambulatory surgery centers across 21 states. As a passionate visionary and innovative problem solver, he has led the changes required for clinical engagement of nearly 2,500 medical professionals and taken the lead on the development of innovative computer systems and technological projects that help NorthStar maintain its leading edge in the healthcare market.
EHC: How many facilities does your group cover, including hospitals and ASCs?
Dr. Woods: NorthStar Anesthesia’s experience includes more than 180 transitions of anesthesia services at individual hospital and surgery center locations. Currently, the NorthStar footprint includes contracts at 143 facilities—approximately 36 of these are ASCs, with the rest being community-based hospitals.
EHC: How many physicians and CRNA’s/AA’s are in your group? What types of models are used at the facilities that you are involved in – CRNA-only models, medically directed or mixture of every type of model?
Dr. Woods: NorthStar’s provider team includes approximately 560 physicians, 1640 CRNAs, and 30 AAs. We are experienced in operating a variety of anesthesia practice models including: 1) physician only models; 2) CRNA only models; 3) physician and care team mixed models; and 4) medical direction models. The vast majority of our facilities currently use a pure medical direction model, a select few use physician-only or CRNA-only models, while the remaining use a model including some form of medical supervision.
EHC: Have you seen an increase in the practices that are under medical supervision?
Dr. Woods: We really haven’t seen a shift in facilities moving to a medically supervised model. Our mantra has always been “local law prevails.” A common misperception for NorthStar and other anesthesia management groups is that we come in, fire a bunch of physicians and hire a bunch of CRNAs to stretch the models. In reality, that has never been our approach. We work with each facility to identify and implement the model that optimizes patient outcomes, improves efficiencies, reduces costs, and adheres to applicable regulations. This usually results in our matching what the facility had before our partnership. Our average supervision rate across all of our facilities is 1:2.8, and we normally employ a medically directed model.
EHC: You use a lot of physician extenders. How do you manage the relationship with them and establish alignment with group objectives, whether they are efficiency objectives and/or clinical objectives?
Dr. Woods: I think this is a key differentiator between NorthStar and all other major groups. Our national focus is not on policy or authority, it is culture. As is commonly described in the business world, “culture eats strategy for breakfast.” At NorthStar, we make sure that our culture is inclusive of both physicians and CRNAs, who are both meaningful members of the team and must both be fully utilized and respected in the process. We are not perfect at this, but that is what we work toward—and when we succeed, the best results follow. It is about establishing mutual respect and inviting great clinical providers, CRNAs and Anesthesiologists, to contribute to the best of their abilities in communication, leadership and clinical care. That is how we focus our teams on the right results in order to get the best patient outcomes.
EHC: When you compare yourself to the other large vendors across the country, what do you view as your competitive advantage?
Dr. Woods: I would put it in this order – Number one: Aligned leadership. Number two: Measuring and managing our patient outcomes. We call it the perioperative continuum, and it is our clinical quality focus. Number three: Being privately held. I think one of the things that sets us apart from all the major groups that are publicly traded is that we are still privately held. In 2018, a long-term capital partner, The Cranemere Group, purchased a majority ownership in NorthStar Anesthesia. What Cranemere has done is shift our thinking from how we move the needle on a quarterly finance report or how we move earnings to a certain point for investors over the next 24 or 36 months to asking what investments we need to make now to have a long-term, sustainable growth company over the next 20 years. That conversation in the board room, at local leadership meetings, and with our partners at local facilities changes the game. We are focused on talking about leadership investments, technical IT investments, and infrastructure for reporting and taking care of patients. The nature of the conversation is radically different when you are talking about a 20-year run versus a two-year run. In our new model, return on investment isn’t required to show up two years from now—it can come in six years, as long as it planned and projected.
EHC: So NorthStar has no plans to go public in the future?
Dr. Woods: Vincent Mai, founder of The Cranemere Group, and Jeff Zients, a former Chief Economic Advisor for President Obama and Director of the Office of Management and Budget, now steer the direction of NorthStar. Cranemere operates with a long-term vision in mind, that “good companies should be held, not sold.” With this new roadmap, our expectation is that NorthStar will focus on long-term sustainable growth and achievement of strategic goals.
EHC: Is NorthStar Cranemere’s first foray into hospital-based physician groups or have they been involved in other specialties?
Dr. Woods: They certainly come from a long history of healthcare investment and healthcare management positions. Jeff Zients was one of the early leaders of the Corporate Executive Board and the Advisory Board, a healthcare think-tank. Through this experience, along with his time with the Obama administration, Zients has a keen appreciation of and expert knowledge in the healthcare industry. NorthStar is Cranemere’s first healthcare investment—in the short time with this relationship, we have already begun to initiate many positive changes within our organization.
EHC: Describe the use of technology in your practice.
Dr. Woods: We leverage technology as much as we can for clinical and documentation purposes but of course we are beholden to the local facilities for their choice of whatever electronic health records they want to employ. Some of the biggest systems right now are Cerner, Epic, All Scripts, etc. What we’ve done is chosen to be AIMS agnostic – meaning we don’t care as much about what the AIMS is in place, we care more about the post-case reporting abilities. As a result of this initiative we’ve gone enterprise-wide with an ePreop solution called Anesthesia Valet. We’ve been partnering with them for about eight years and this partnership facilitates our quality collections on the backside of case performance. We are now beginning implementation of the SurgicalValetTM, suite which is the front-end of perioperative care via PAT improvements and coordination at several of our facilities. In addition to our primary technological investment through vendors and partnerships we also have our own proprietary scheduling and manpower utilization systems, as well as our analytics and practice management suites that we’ve been building for the last 14 years.
In the clinical space, we now play with a lot of different clinical monitoring processes specifically around hemodynamics, enhanced recovery, and goal-directed therapies. This adds to our ability to monitor and be accountable to our inputs to patient care paths, so we can measure the output and outcomes.
For our providers, over the past few years we’ve moved most of our CRM and our relational connectivity to the providers to mobile platform applications. Just about everything you need to do to interact with the company, with HR and with all the other departments like payroll and benefits has been moved into these mobile applications platforms so that it is easy for them when they are in between cases or moving around their busy clinical facilities.
EHC: What metrics do you use to track performance (for example – AQI, hospital quality dashboard, surgeon satisfaction, patient satisfaction, on time starts, post op pains scores etc.)
Dr. Woods: We measure most of the common metrics in the clinical environment that everybody else is chasing. Most of those are tied to what we are doing with our submissions through the ePreop QCDR, and then up to the AQI where we follow the same ASA recommendations that everybody else does. In addition, we usually have between six and ten individual performance or outcome metrics in our facility contracts, which are chosen by our facility partners. These range from first-case on-time starts (FCOTS) to turnover times (TOT) to post-documentation of the 48-hour follow-up required by CMS.
We are also building out a new expansive look at our manpower utilization and productivity for physicians, CRNAs and AAs and looking at the best ways to monitor how we are doing managing our people and their time in the facility. This one is very important for us long-term and for the good of our people to be able to document the amount of hard work that’s being done and use that as a leverage point in our provision of care for growing surgical volumes.
EHC: Another issue especially for a group that works in so many facilities and has such a wide geography, is maximizing your revenue cycle performance. How do you monitor and track that, and get it back on track if there are ever deviations?
Dr. Woods: We’ve had tremendous improvement in our RCM process management and output. We’ve raised our blended unit rate collected per unit by almost 21% over the last year and a half. That is attributable a lot to Ashwini Kotwal, our CFO. She has been magnificent working with our major revenue cycle vendors and has helped our billing companies become more efficient in their own processes and made our processes more efficient in getting the information to them. Because of that, negotiation of rates has shown tremendous improvement. This year our focus is on two fronts – One: using our scale and geographies in various areas to align and drive our discussions with our third-party payors. And two: measurement in our reporting data for performance and production at the individual provider level. We are trying to aid our providers through education and more individual accountability for what they’re documenting in their care and what they may be missing.
EHC: What are your strategic objectives for the next 2 to 5 years?
Dr. Woods: Our strategic objectives surround a continued focus on our RCM rate negotiations and processes, reestablishing our organization’s culture, and smart sustainable growth. Our growth will largely be organic in nature (with which NorthStar has a long-standing history). Additionally, we look forward to a renewed focus on growth related to strategic mergers and acquisitions.
EHC: Thank you very much Dr Woods. We appreciate your time and insight today

Dr. Robert Stiefel is a board-certified anesthesiologist and co-founder of a major anesthesia practice management company that operated across 27 facilities. With over 20 years of experience as a clinician and consultant, he is a national leader in understanding anesthesia expense drivers. He has led initiatives in group governance, subsidy negotiations, compensation models, and policy development. For more than 16 years, he has consulted professionally and co-founded Enhance Healthcare with Dr. Greenfield. Dr. Stiefel earned his MD from Tufts and completed his residency at the University of Massachusetts.